Big aspirations, small budgets - and disenfranchised mental health care patients
By Elena Sosa Lerin and Lucas Bottoman
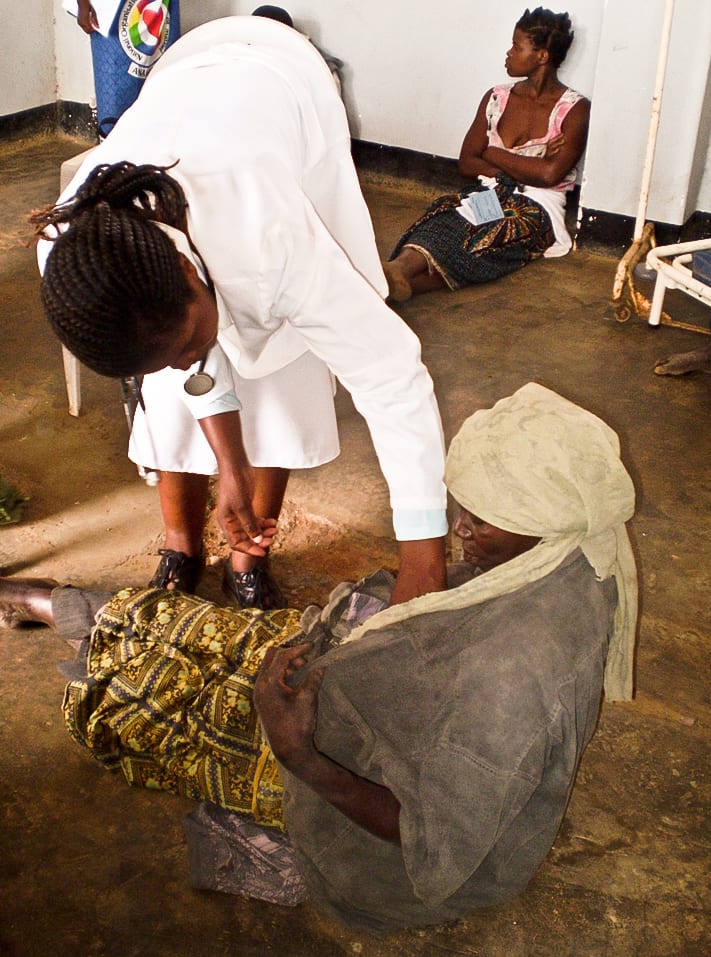
Epilepsy, depression, schizophrenia and bipolar disorders are some of the top mental health issues in Malawi. Photo: Courtesy of Blantyre News Limited
The World Health Organization (WHO) reports mental health issues are already the fourth leading cause of the global health burden, representing a third of all years of healthy life lost to disability among adults.
By 2020, they will rank second, behind heart disease.
WHO studies indicate that in Africa, mental health issues such as epilepsy, depression, psychosis, substance abuse, and other psychotic disorders are among the top ten causes of disability.
But in Malawi, where health policies and development goals are primarily centred on the prevention of HIV and AIDS, the reduction of maternal mortality, tuberculosis, and malaria, mental healthcare is — at best — an afterthought.
Case in point, the Ministry of Health has no reliable data on the nature and the extent of those suffering mental disorders.
Its National Mental Health Policy Plan admits that it has had to rely on studies done in neighbouring countries in the absence of national research on mental health patients.
Based on these studies, health officials estimate that at least ten percent of Malawi's 15 million people are affected by a mental health issue, meaning that mental health disorders are as common as infectious diseases.
And yet, given these dire statistics, the Ministry of Health's Strategic Plan for 2011-2016 recognizes that the government's budget for the health sector is "inadequate."
Health places third in budgetary allocation (at 10.2 percent) after education (13.7 percent) and agriculture (18.9 percent).
Less than two percent of the national health budget is spent on mental health care.
In 2007 and 2009, respectively, Malawi signed and ratified the United Nations Convention on the Rights of Persons with Disabilities and its Principles for the Protection of Persons with Mental Illness and for the Improvement of Mental Health Care.
Among the guiding principles of this Convention are accessibility to facilities and services, the right to health, as well as habilitation and rehabilitation services and programs.
The Malawian Constitution addresses the right to development, declaring that the State commits itself to "take all necessary measures" to guarantee "access to basic resources, […and] health services."
But with such a tight budget, intentions can only go so far.
People with a mental health condition have to deal with public mental healthcare institutions that suffer chronic shortages of essential drugs, inadequate if not, deteriorating facilities, insufficient and overworked nurses and doctors, and no counselling access.
For instance, the psychiatric section of the Queen Elizabeth Central Hospital (QECH), the largest hospital in the city of Blantyre, has been out of essential drugs (like Chlorpromazine and Modecate, used in the treatment of conditions such as schizophrenia, psychoses and manic episodes) for over a year. Bwaila Hospital in the capital, Lilongwe, has lacked medication for ten months.
Based on hospital records, six out of ten patients are relapsing due to the lack of drugs at QECH.
"There's no hope for many patients," says one of the psychiatric nurses from QECH. "It is a very sad situation to see — and we can't do much about it."
The little the nurses can do is to substitute drugs if possible. But sometimes, they have to turn patients away if they don't have the right drugs to treat their specific needs.
"We feel very sorry to tell the patients who have walked for many hours to get their medication that we don't have any," says another nurse from Bwaila Hospital.
Adding to the lack of essential drugs, there's also the scarcity of mental health care workers.
For instance, QECH has just one psychiatrist and 18 nurses to attend an average of 2,700 patients a year. Bwaila Hospital doesn't even have a psychiatrist. It's entirely run by five nurses who attend about 200 patients every day.
Two years ago, Dr. Rob Stewart, the head of the psychiatric unit at QECH, decided to shut down patients' admissions because the rooms lacked windows and toilets.
One of the nurses from QECH, when asked what improvements she'd like to see in the mental health care system, said having a computer would make a big difference, as patients' records are still handwritten and usually get lost or mixed with other papers.
"The only piece of technology we have here is a telephone," she says.
► A version of this story was originally published on September 2011 in The Toronto Star's 'Africa without Maps' blog.
Follow me on Twitter: @e_sarin. Email me your thoughts, suggestions, or critiques at: elenasosalerin@gmail.com.